Tarsal Tunnel SyndromeTarsal Tunnel Syndrome (TTS) is a nerve disorder caused by the compression or damage to the posterior tibial nerve. This tendon is located in your tarsal canal, which runs through a small space along the inside of your ankle into the heel and sole of your foot. This condition is slowly progressive and occurs more commonly after 30 - 40 years of age. It causes a lot of pain in your foot, ankle and toes. 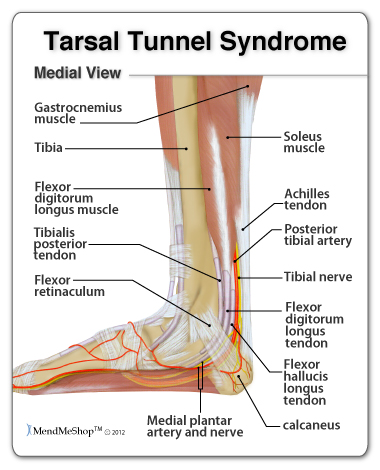 Often damage to your posterior tibial nerve in one location affects the overall functioning of your nerve, so you are more at risk of suffering from compression in other areas along the nerve. The nerve sends signals along its length and also carries its own nutrients, which are necessary for optimal function. Nutrients move along the entire length of your nerve via axoplasms (jelly-like material that fills the axons). If the flow of these nutrients is blocked, your nerve tissue further from the area of compression does not receive the essential nutrients to fight off injuries, and damage, pain and inflammation will get worse. Similar conditions and other names for tarsal tunnel syndrome include: tarsal tunnel neuropathy, entrapment neuropathy of the tibial nerve, posterior tibial neuropathy, compression of the tibial nerve, and posterior tibial neuralgia. Tarsal tunnel syndrome (TTS) is similar to carpal tunnel syndrome, which occurs in your wrist, however it is far less common. Anatomy of the Tarsal TunnelThe tarsal tunnel is found between the thick, overlying fibrous tissue on one side of your foot and the underlying bones. The flexor retinaculum acts as the top of your tarsal tunnel. It forms a deep, band of fibrous connective tissue that surrounds the muscles and nerves in your lower leg and ankle. The top of the calcaneus (heel bone), the inner wall of the talus (2nd largest tarsal bone that forms the ankle joint connecting the leg bones to the foot bones) and the inner/bottom part of the tibia (shinbone) comprise the bottom of your tarsal tunnel. Your ankle tendons, nerves, arteries and veins pass through the tarsal tunnel to get to the bottom of your foot. The posterior tibial nerve is found between the posterior tibial muscle, the flexor digitorum longus, and the flexor hallucis longus muscles in your lower leg/ankle. The tibial nerve moves behind the bump on the inside of your ankle (medial malleolus) and through the tarsal tunnel, where it then divides into nerve branches in the sole of your foot. Causes of Tarsal TunnelAny compression or entrapment of the posterior tibial nerve in the tarsal tunnel can cause tarsal tunnel syndrome. This may occur with: 
Symptoms of Tarsal TunnelAlthough they vary from person to person, most of these symptoms are generally experienced on either the inside of the ankle and/or the bottom of the foot. The most common symptoms noted by those who suffer from Tarsal Tunnel Syndrome are:
You can feel these symptoms on their own in one location or in various locations across your foot and lower leg. They can be aggravated by overuse of your foot through walking, exercising or prolonged standing. These symptoms will often subside with rest however they will not disappear. If left untreated, you are at risk of suffering from permanent nerve damage. Tarsal Tunnel Treatment OptionsThe most important factor in dealing with Tarsal Tunnel Syndrome is resting your ankle. This can be difficult when you have to carry on with daily activities, but resting and elevating your foot whenever you can is recommended. During your recovery you will probably have to modify or avoid the activities that put stress on your ankle until your pain and inflammation settle. Although steroid injections may provide temporary relief from the pain of an a soft tissue injury in the achilles and heel, they should generally be undertaken with caution as they weaken strained tendons... and may lead to a complete rupture. If you do opt for an injection, doctors usually recommend that you do not participate in strenuous activities for several weeks to reduce the risk of a rupture. Conservative Treatment Step 1: Reduce The Initial InflammationInflammation is often a causal factor with tarsal tunnel, and is often a response to an immediate ankle injury and is a normal part of the healing process - helping to reduce tissue infection in the early stages of injury. Swelling, pain, heat sensation, redness, and loss of function are the main symptoms experienced. Cold Compression will reduce pain, inflammation and swelling in your ankle to treat tarsal tunnel causes and symptoms. Note that the importance of the cold is very high, though when surveyed, most TTS sufferers never take advantage of this easy treatment step. By limiting the amount of damage done to your posterior tibial nerve, you also reduce pain and limit the amount of healing that needs to occur. This is a very important step to get rid of tarsal tunnel syndrome faster and with less pain! Applying cold to your affected ankle will decrease the swelling and redness at the injury site. In addition, it will numb the pain in your ankle and help to control the inflammation. Simply, apply cold to your ankle as needed throughout the day, for approximately 10-15 minutes at a time. The combination of rest, topical pain relief cream and cold is the gold standard in medicine for minimizing tissue damage, reducing heel pain and reducing inflammation after injury or activity. Conservative Treatment Step 2: See Your Physician & Physical TherapistYour physical therapist will most likely assess your specific biomechanics and attempt to correct them if they are determined to be causal factors to your condition. Further to this, some causal factors may require surgery so it is important to get to your doctor and have it checked out. Stretching and strengthening exercises, centered on the lower leg and ankle will probably be assigned to you by your physical therapist as well. Conservative Treatment Step 3: Enhance Blood Flow (via Deep Heat) to the AnkleOnce the inflammation in the achilles and lower leg have been reduced, nourishing and strengthening the injured soft tissue is recommended. Conservative Treatment Step 3:
|

Achilles Tendon Facts There are over 250,000 achilles tendon injuries each year in the US. Achilles tendon ruptures are common in people between the ages of 30 and 50. In runners, too rapid an increase in mileage, hill training without proper strengthening, and recent or inadequate changes to running gear can cause injuries to the Achilles tendon. Achilles tendonitis accounts for an estimated 11% of running injuries. 3-5% of athletes are forced to leave their sports career due to Achilles tendon overuse injuries that go untreated. Medications mask the pain but do very little in the healing of Achilles tendonitis. A fully ruptured tendon REQUIRES surgery. It will not heal on its own. Achilles tendonitis and Achilles tendinitis are the same thing. Continually using your Achilles tendon while it is injured will lead to a more serious and/or chronic injury.          |



