Anatomy of the AchillesAnatomy of the Achilles TendonThe Achilles tendon, also known as the calcaneal tendon, is a white fibrous cord located at the back of the ankle. Essential in the flexion of the subtalar joint (also known as the talocalcaneal joint) in the ankle which exists between the calcaneus (heel bone) and the talus bone. Contracting your calf muscles forces the tendon to lift your heel. By flexing your calf or leg muscles, your Achilles is activated and your foot pushes down. This is how you are able to create movements such as walking, running, and jumping. If your Achilles Tendon is injured, everyday movements like walking, jumping and even standing can become painful or maybe even impossible to do! Tendons connect muscle tissue to bone. The Achilles tendon connects the calf muscles (gastrocnemius and soleus muscles) and to the heel bone(calcaneus). Heel bones can very in shape and size from person to person. An irregular shape heel (calcaneus) can cause the Achilles tendon to twist or a smaller heel bone will put additional stress on Achilles tendon. Achilles Tendon - What is it Made From?The Achilles tendon is made up of strands of protein called collagen that run parallel to each other and are bundled closely together within the Achilles tendon. The smallest collagen component is called a collagen fibril or tenocyte. These small strands are bundled together within a collagen fiber. Several collagen fibers are bound together and make up the next layer within the tendon called the fascicle. The fascicle, combined with the subfascicles, form 3 different levels of collagen. These levels are referred to as the primary, secondary and tertiary fiber bundles. The endotenon surrounds the fascicle to stabilize and bind them together within the Achilles tendon. The endotenon are then bound together by the final layer of the tendon, called the peritendon, which is made up of 3 layers as well. The epitenon is the interior layer, closest to the endotenons which contains the vascular, lymphatic, and nerve supply. 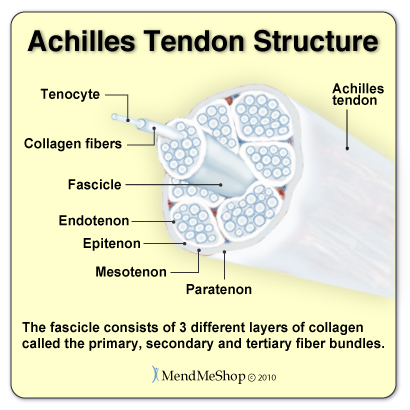 Next is the mesotenon which is filled with a thin, lubricating fluid that allows for the Achilles tendon to glide when the gastrocenemius and soleus muscles in the calf contract. The paratenon is the outer layer binding all of the Achilles tendon together and is part of the deep fascia that runs throughout your entire body. Unlike other tendons in the body, the Achilles tendon does not have a true synovial sheath covering it, rather it is surrounded by this loose outer covering of fatty tissue. Although tendons contain blood vessels and nerves, compared to other parts of the body the Achilles tendons have a very poor supply of blood. They receive the least amount of blood between 3/4" and 2 1/2" above where the Achilles tendon attaches to the calcaneus heel bone making this area the weakest part of the Achilles tendon and the slowest area to heal. Stress on the AchillesWith each step, your Achilles tendon supports the weight of your entire body. Depending on your speed, the length between your steps, and the ground beneath you, your Achilles could be supporting 3-12x the force of your body weight! In a study of the functional anatomy of the Achilles tendon, participants experienced 12.5x the force of their body weight exerted on their Achilles Tendon while running! That means that your tendon has to be able to support extreme amounts of pressure on a daily basis! In order for your Achilles Tendon to perform the task you need it to, it must be strong and healthy. Nourishment for your tendon is provided by good circulation of your blood. Blood for your Achilles is provided by two arteries. These arteries pump blood through the calf muscles and the bone interfaces which transfers blood to your tendon. Unfortunately, this means that only PART of your tendon is receiving steady, consistent blood flow. The circulation where the Achilles meets the heel bone is very weak. Blood supply to the area in your tendon 3/4-2/12" above the Achilles-Heel connection has the lowest blood supply. Grades of Tendon StrainsLike any tendon strain, an achilles tendon strain can be classified depending on the severity of the strain. Strains can vary from a small discomfort with over stretching the muscle to a full rupture. Grade 1 - Mild StrainA 'Grade 1' strain feels more like a discomfort in lower back of the leg as opposed to acute pain. With a grade 1 strain there is some stretching or minor tearing of the tendon and/or surrounding tissue. These injuries usually respond quickly if treated properly with conservative treatments such as a Cold Compress or Ice Pack and an Achilles TShellz Wrap®. Grade 2 - Moderate StrainA 'Grade II' strain is an actual partial tear in the muscle or the tendon. It would feel like a sharp pain within the achilles, perhaps even accompanied by a tearing sound. A grade 2 strain occurs when a tendon or muscle is partially torn but still intact. If you have a grade 2 strain, strength is noticeably reduced. Your physician may decide on surgery or a conservative treatment protocol, depending on your specific situation. Grade 3 - Rupture or Severe StrainA 'Grade III' tear is typically signified by a very sharp pain within the achilles at the time of the injury. Some say the feeling is like getting a kick in the calf muscle. There is also a significant amount of pain when attempting to push off on the injured leg when walking - in cases of complete rupture, you will not be able to push off your leg. The stability of the ankle is greatly reduced and pain and swelling is typically evident. Treatment of a Grade 3 tendon injury usually requires surgery to rejoin the tendon back to the muscle or bone where it has become severed (or substantially torn). Achilles BursaeBursae = Plural form of Bursa 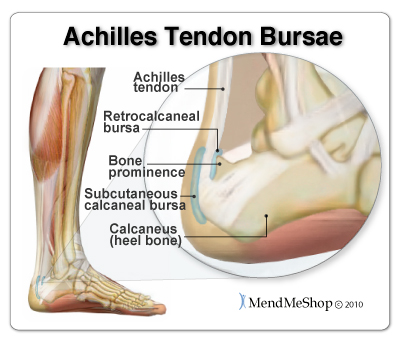 Bursae are sacs that are lined with synovial tissue. These sacs provide cushioning between tissue and bone where needed throughout the body. There are 2 bursae located near the insertion of the Achilles tendon at the heel bone, the retrocalcaneal bursa and subcutaneous calcaneal bursa. The retrocalcaneal bursa lies between the Achilles tendon and the back, surface of the heel bone (calcaneus). This is a "true" bursa that is present from birth. The larger subcutaneous calcaneal bursa lies overtop of the tendon at the lower part of the heel where the Achilles tendon joins to the heel bone. This bursa develops as you age (called an "adventitious" bursa) to protect the tendon from friction that can damage soft tissue. Healing the Achilles TendonThe heel of the foot is a small area with a lot going on, the Achilles tendon attachment, the bursa sac (lubricates the joint), the plantar fascia ligament (under your foot) and the fat pad under the heel.
All can become irritated, this can be the challenge to heal the tendon and could lead to chronic Achilles conditions. Your damaged tendon fibers can harden (become calcified). This extra calcium can gather where the Achilles tendon is under stress resulting in a bone spur.
If your Achilles tendon is injured and you continue to stretch and strain it, tough and inflexible scar tissue will replace the Achilles tendon's normally elastic fibrous tissue. The unhealthy tissue now in place hurts during exercise, is more likely to further degrade, and can become a constant pain even while you walk. An Achilles tendon injury or tendonitis (also spelled tendinitis) that is left untreated can become a chronic condition that is extremely troublesome to cure. So, if your Achilles is injured, it's important to treat it and heal as fast as possible. Unfortunately, an Achilles tendon is dense and fibrous with limited blood vessels which does not allow for ample blood flow. As a result, the Achilles tendon heals slowly by nature. The trick to treating any tendon injury is getting it to heal quickly, with minimal scar tissue formation, and with as much proper realignment of the tendon fibers as possible. By healing your Achilles tendon tissue faster and more completely, you maintain more elasticity in the fibers. A more elastic tendon is less prone to further pain and injury than a tight, unhealthy tendon that is held together with scar tissue. Achilles Strengthening & SupportYour legs support an intense amount of weight every day! In order to handle the pressures put on them, you must keep your muscles and tendons strong. Use stretching exercises - assigned by your physical therapist (PT) - to increase strength and flexibility of your leg with smooth controlled movements. You can start out small and increase at your own, slow but safe pace. Minimize your chance of re-injury and decrease your time spent in pain and discomfort. Your full recovery depends on your commitment to stretching and strengthening exercises. Your PT will develop an effective program during your clinic visits for your recovery. But ask any PT, the key to a successful recovery is commitment to at home exercise! Learn More About Achilles Injuries & TreatmentsI want to learn more about Achilles Surgery & Post-Surgery Recovery I want to learn more about Circulation Boost I want to learn more about Ice & Heat: Which Is Better For The Achilles? I want to learn more about Stretching for the Achilles FREE SHIPPING ON ALL PRODUCTS CURRENTLY ENABLED |

Achilles Tendon Facts There are over 250,000 achilles tendon injuries each year in the US. Achilles tendon ruptures are common in people between the ages of 30 and 50. In runners, too rapid an increase in mileage, hill training without proper strengthening, and recent or inadequate changes to running gear can cause injuries to the Achilles tendon. Achilles tendonitis accounts for an estimated 11% of running injuries. 3-5% of athletes are forced to leave their sports career due to Achilles tendon overuse injuries that go untreated. Medications mask the pain but do very little in the healing of Achilles tendonitis. A fully ruptured tendon REQUIRES surgery. It will not heal on its own. Achilles tendonitis and Achilles tendinitis are the same thing. Continually using your Achilles tendon while it is injured will lead to a more serious and/or chronic injury.          |



